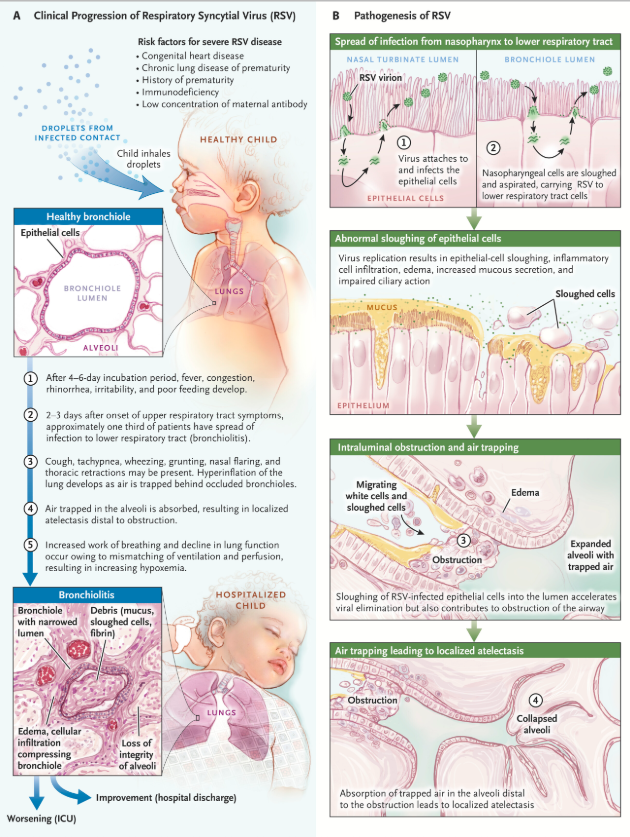
Bronchiolitis is an extremely common lower respiratory tract infection in infants and young children. Symptoms can include fever, coughing, and signs of lower respiratory tract obstruction such as tachypnea, nasal flaring, belly breathing, retractions, head bobbing, and in young infants, apneas.
Epidemiology
Bronchiolitis is the most frequent cause of hospitalization for respiratory illness in infants under 12 months of age, with rates of hospitalization peaking in infants between
2–6 months of age. Bronchiolitis is technically a diagnosis applied to young children < 2 years of age. However this is more semantics as children >2 years of age often get lower respiratory tract viral infections with the same underlying pathophysiology as is seen in bronchiolitis but as their airways are technically slightly larger after 2 years of age the label of bronchiolitis is not applied. Children over 2 years of age with lower respiratory tract infections are also less likely to require admission to the hospital.
There is a strong seasonal association with bronchiolitis as viral respiratory pathogens increase/peak during fall and winter, often running from October through March in the northern hemisphere.
It is noteworthy that at the height of the COVID pandemic from fall 2020 through summer 2021, there was a significant drop in cases of bronchiolitis when infection control measures were being carefully adhered to by a large segment of the U.S. population. Then in 2021 and 2022, there was a major resurgence in respiratory syncytial virus (RSV) infections and other viral respiratory infections beginning earlier than expected. In 2023, the pattern of these infections settled into a pattern more similar to seasons prior to the COVID pandemic.
Etiology
Bronchiolitis can be caused by any viral pathogen, with RSV being the most common and most publicized during the classic fall/winter season and rhinovirus being the most common in the off season.
Pathogenesis and pathophysiology
Bronchiolitis occurs when viruses infect the bronchiolar epithelial cells of the terminal airways, causing subsequent inflammation and direct cytotoxicity to bronchioles in the lungs. The virus attaches to the epithelial cells in the bronchioles and replicates. The inflammatory response leads to edema and increases mucous production, both of which obstruct airflow through the bronchioles. Microscopic inspection of the pathology from prior studies demonstrates bronchiolar cell necrosis, ciliary disruption, and peribronchiolar lymphocytic infiltration. See Figure 1 below.
Clinical features
A cough is often the first symptom and is typically accompanied by other symptoms of viral respiratory infection including fever, nasal congestion, and active rhinorrhea. The lung exam in bronchiolitis can be varied, most commonly consisting of low-pitched sounds (rhonchi) and non-fixed wheezing but can also include crackles and overall poor aeration. Wheezing that is not fixed is due to mucous plugging, which differentiates it from the wheezing in asthma that is related to bronchoconstriction.
When assessing a child with lower respiratory infection it is important to listen multiple times throughout your exam. Having them cough, cry, or scream can mobilize mucous and aid in differentiating whether there are more fixed obstructive processes (that would increase your suspicion for pneumonia) or fixed wheezing (that would increase your suspicion for underlying bronchoconstriction).
Respiratory distress is stratified into mild/moderate/severe and includes signs such as increased respiratory rate (for age), grunting, nasal flaring, head bobbing, belly breathing, retractions visible in the intercostal, subcostal, and suprasternal notch regions, hypoxia/cyanosis, and apnea.
Risk factors for developing more severe distress
- Young age (< 6 months). Newborns < 4 weeks are the highest risk for apnea.
- History of prematurity.
- Chronic lung disease or known history of bronchopulmonary dysplasia.
- Unrepaired congenital heart disease with known shunting.
Diagnosis
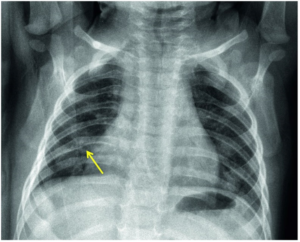 The diagnosis of bronchiolitis is clinical (based on the patient’s history and physical examination). Laboratory testing and radiographic studies are not recommended for diagnosis. CBC, inflammatory markers, blood culture, and chest x-ray should only be used when a serious bacterial infection (SBI) is suspected. A viral respiratory panel may be used to aid in the more accurate diagnosis of the viral pathogen, which may be useful for the hospitalized patient or in patients not following the expected course of illness. A chest x-ray may be performed to rule out conditions like effusions or pneumothorax when there is clinical suspicion but should not be used to evaluate for pneumonia as that is a clinical diagnosis. In bronchiolitis, the chest x-ray may show hyperinflation of the lungs, atelectasis, or peribronchial cuffing that is often referred to as the classic cheerio (see CXR).
The diagnosis of bronchiolitis is clinical (based on the patient’s history and physical examination). Laboratory testing and radiographic studies are not recommended for diagnosis. CBC, inflammatory markers, blood culture, and chest x-ray should only be used when a serious bacterial infection (SBI) is suspected. A viral respiratory panel may be used to aid in the more accurate diagnosis of the viral pathogen, which may be useful for the hospitalized patient or in patients not following the expected course of illness. A chest x-ray may be performed to rule out conditions like effusions or pneumothorax when there is clinical suspicion but should not be used to evaluate for pneumonia as that is a clinical diagnosis. In bronchiolitis, the chest x-ray may show hyperinflation of the lungs, atelectasis, or peribronchial cuffing that is often referred to as the classic cheerio (see CXR).
-
Assessing severity
There are multiple ways to score severity of respiratory distress in the setting of bronchiolitis, which in turns aids in informing how aggressive clinical management should be and whether hospitalization should be considered. Most large Children’s Hospitals have internal scoring systems; however, they often include the following consistent variables: Respiratory rate based on age, work of breathing, mental status, oxygen requirement, and breath sounds.
One such scoring system is the Respiratory Severity Score (RSS):
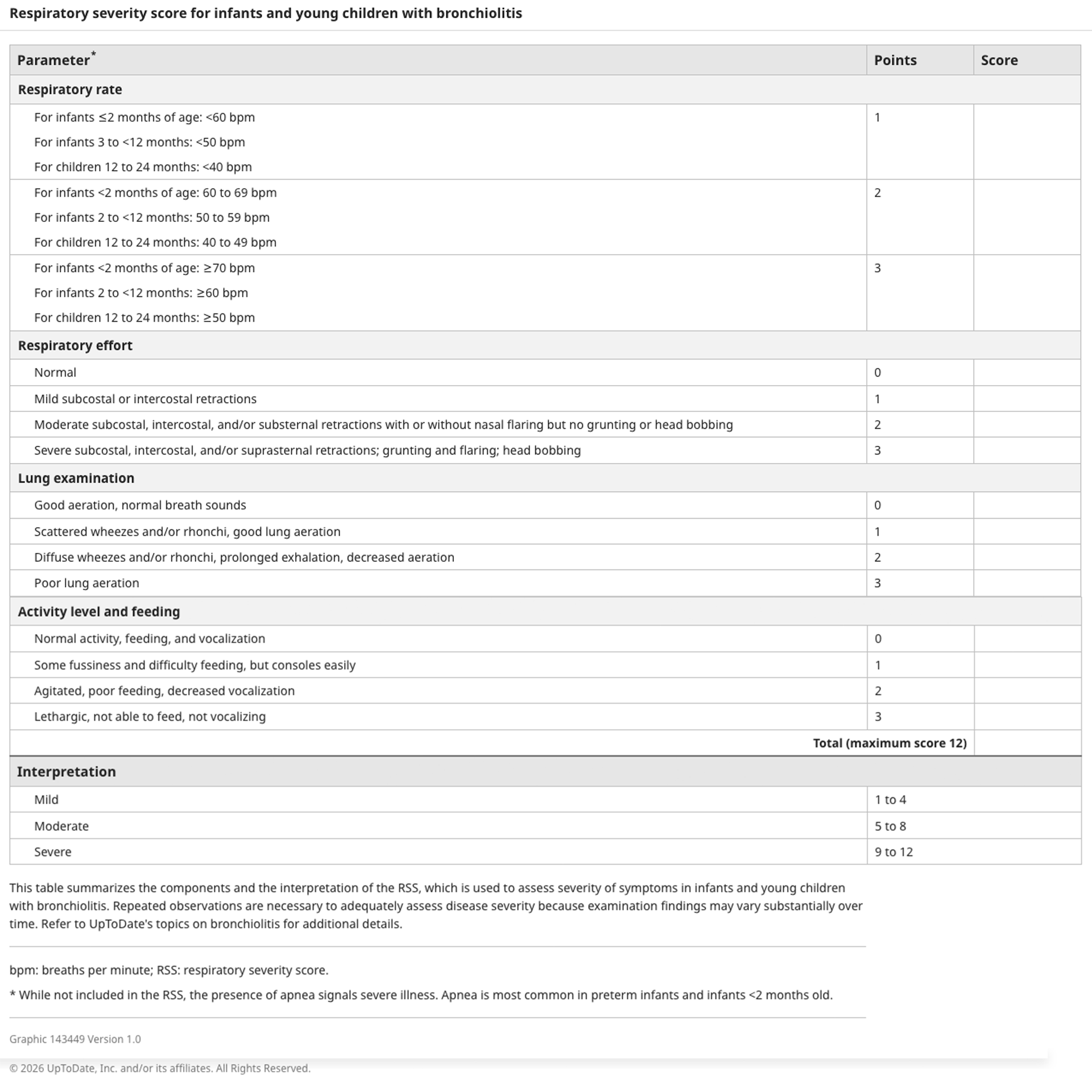
While these scoring tools aid in management decisions at initial presentation, decision to admit should also take into account whether the patient is able to hydrate well on their own and where they are in their illness course (as we know most viral infections will worsen until their 3–5 day peak and then start to self-resolve). If the family lives very far from their nearest healthcare facility, or cannot get close follow up with their pediatrician, the provider may also make the decision to admit the child for close monitoring.
Treatment
The mainstay of treatment for bronchiolitis is suctioning to clear secretions, which can be done at home with something such as the Nose Frieda, or in the clinic/hospital setting with off the wall suction. Bulb suction tends to be low yield as it is too superficial to address the majority of the upper airway secretions causing partial obstruction. Parents may be instructed to use nasal saline when suctioning for better clearance.
Hospitalized children may require further support with supplemental oxygen (often simple nasal cannula), positive pressure supports (high flow nasal cannula, CPAP, or intubation), and IV fluids. Prior to initiating respiratory support the patient should always be suctioned to optimize penetration of the oxygen or pressurized air. A nasopharyngeal suctioning can be high yield to clear out the dead space in the posterior oropharynx.
Bronchodilators (albuterol) and corticosteroids are used only if there is a reactive airway component (history of asthma or high suspicion for new asthma diagnosis based on presentation). Hypertonic saline nebulization is no longer recommended as multiple studies have shown low utility.
Patients with worsening respiratory status may require escalating respiratory support with PICU admission.
Prevention
Given that bronchiolitis is primarily caused by viral pathogens, preventive strategies focus on minimizing the risk of viral transmission. Hand hygiene remains the cornerstone of prevention, with soap and water the most effective strategy but alcohol-based hand sanitizers being a viable option when hands are not visibly soiled. Masking when ill is another evidence-based measure to reduce the spread of respiratory pathogens that can cause bronchiolitis, particularly in high-risk settings or during peak viral seasons. Parental education is critical, especially regarding the role of vaccination in lowering the risk of secondary bacterial complications from bronchiolitis but in primary prevention of initial disease through immunization against influenza and COVID-19.
Specifically, regarding RSV, discussion with family should be had regarding the monoclonal antibody Niresevimab (Beyfortus) which offers protection for infants through their first (and in high-risk children also their second) RSV season. Use of the maternal RSV vaccine in the 32nd thru 36th week of pregnancy also offers significant protection to baby, and these vaccines are offered to pregnant mothers from September through January. If a baby’s mother was able to get the vaccine, then the child does not need to get the monoclonal antibody. Prophylaxis to newborns with palivizumab is no longer recommended by the American Academy of Pediatrics.
Conclusion
Bronchiolitis is one of the most common respiratory infections in infants and young children, leading to a high number of hospitalizations each year. Effective management can reduce healthcare costs and improve resource utilization.
- Meissner HC. Viral Bronchiolitis in Children. N Engl J Med; 374(1). 2016.
- Centers for Disease Control and Prevention. (2024, August). RSV Vaccine Guidance for Pregnant Women.
- Nicholson E, Schroeder A, Piedra PA. Bronchiolitis in infants and children: Clinical features and diagnosis. UpToDate. 2024. Last updated March 10, 2026. Accessed April 2026.
- Schroeder A, Nicholson E. Bronchiolitis in infants and children: Treatment, outcome, and prevention. UpToDate. 2024. Last updated: March 9, 2026. Accessed April 2026.
- Ralston SL, Lieberthal AS, Meissner HC, et al. Clinical practice guideline: the diagnosis, management, and prevention of bronchiolitis. Pediatrics November 2014; 134 (5): e1474–e1502.
Image credits
Unless otherwise noted, images are from Adobe Stock.